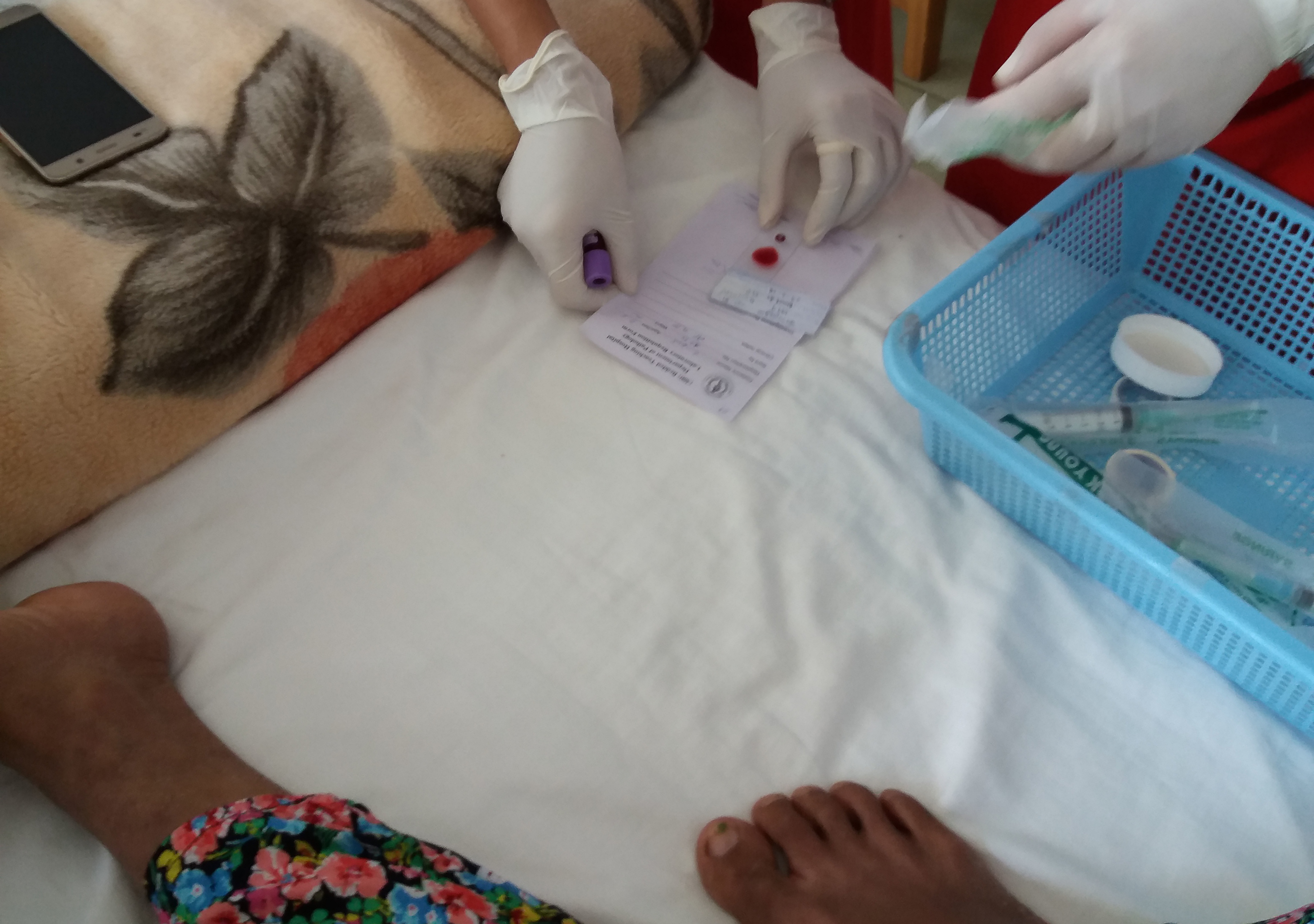
With the COVID19 pandemic affecting lives everywhere around the world, global differences in health care were often mentioned as one of the most concerning aspects in meeting this challenge. Jella Fink shared her observations of social practices around health care in Myanmar’s hospitals in an article in Sojourn: Journal of Social Issues in Southeast Asia last year. Her personal impressions stem from supporting a close friend.
Spending time in a Myanmar hospital was certainly not at the top of my bucket list. Being in the ward as involuntarily as everyone else, I came in as an uninformed friend. As a member of the group of caregivers, I automatically became a participant observer of Myanmar’s hospital culture (anthropological habits die hard), and tried to collect as much intelligence as possible to support my friend’s recovery.
The ward we ended up in after a hazardous journey to several physicians is a typical ward of a government-funded hospital in Myanmar. Basic services are available for free, whilst additional costs for medicine, some laboratory tests and food must be borne by the patient. Private hospitals are available but remain unaffordable for most people. And while basic health insurance has recently become available, it only covers a period of one year, and the available budget per client is limited. Overall, most health-related costs are covered by individuals and their families. If the money runs out, the patient’s recovery is put at stake.

“We Will Wait and See”
“We will wait and see” is a frequently repeated credo in the hospital setting in Myanmar, which expresses the attitude of physicians, patients and their families. The patience and acceptance of fate of Myanmar nationals seem to shimmer through. No matter how bad a patient’s condition is, all processes run quietly here. New patients are settled into their beds, awaiting the physician’s initial checkup.
The noise level is surprisingly low considering the number of people. Every once in a while, however, the quiet is disrupted by the sharp squeaking of the wheels of oxygen tanks being moved back and forth by caregivers. The caregivers are not healthcare professionals, they are the patient’s relatives (rarely, friends), who are present twenty-four hours a day. In this hospital there are many young physicians. They move slowly from patient to patient, not as hurried as I observed at another hospital in Myanmar. The daily examination is followed by a conversation about the patient’s health status amongst physician, patient and caregivers. The physicians are very engaged in determining the patient’s condition. But at times information gets lost, as there is an unspoken consensus amongst caregivers and patients that information that is not asked for specifically will also not be given—and this can include additional symptoms, for example.
Those are then communicated to their relatives, who will decide if that information should be shared with the physicians.
The group of caregivers—the relatives—deserves special attention. It is they who do much of the work, which I—as a Westerner—had only ever witnessed being executed by physicians and nurses. To my understanding, visiting a patient includes bringing flowers and being entertaining company at the cafeteria. But this is not the case at a hospital in Myanmar. Instead, there is a twenty-four-hour shift for caregivers. Most of the time, these caregivers are relatives, either one or two people (husband and child or adult children and their offspring, for example), who spend day and night at the hospital. Their tasks include organizational, logistical and nursing-related
activities. Joking between the members of different families is a way to lighten the mood and pass some time. Discussing the prices of the fruit seller, as well as the offers at different teashops, are the most frequent topics. Medical conditions are not a focal point of discussions.
Waiting and seeing is also covered by extensive smartphone usage. Sometimes, pictures of the hospitalized are taken and shared on social media platforms, like Facebook. This is another example of the differences in understandings of privacy on the one hand and good intentions on the other. By sharing this image the patient may be able to receive positive thoughts/energy from other friends, so-called “metta”, which will support the recovery. Besides this, using phones to watch music videos or playing games is particularly popular—as long as the power bank lasts. Charging via the hospital’s power sockets is prohibited. There are few other activities that are used to busy oneself. The granddaughter of the elderly lady next to my friend’s bed worked speedily on solving two Rubik’s cubes she had brought along. Her mother was not feeling very well that day and was sleeping coiled up on the bench behind the bed. One of the beds in the ward was empty, and so a cat claimed it for its own.

Ward Routines—Developing a New Normal
This ward is made of a large, open room divided by chest-high walls into four equally sized partitions. Each space contains six beds, each with a worn-out nightstand next to it. In this setting, privacy is no longer a given. Examinations are sometimes concealed by a movable partition. But when a new patient comes in, this is not the case. Under the observing eyes of the whole ward, the new patient is brought in and the upper body undressed for auscultation. In some hospitals the ward is divided by gender, but not here. The same conditions apply to anyone needing a chamber pot. The hospital is equipped with old metal bed frames, which are topped with a thin blue plastic-foiled mat for basic comfort. The practices on how to use and how not to use the bed are very specific. Most importantly, another person should not sit on the patient’s bed. But the absence of a table seems to render it an acceptable substitute: an old piece of fabric is spread out with pots and plates placed upon it to enjoy meals together. On the first day, curry dishes brought from home may still be available, but after that—as their caring tasks span the whole twenty-four hours of the day—everyone needs to rely on the food provided by teashops nearby. The purchased food is brought back in plastic bags, which are then carefully draped in the metal pots. In this way, only the two or three plates that have been eaten off need to be washed in the sole bathroom sink shared by the whole ward. Needless to say, this influx of foreign household items and foodstuffs does not improve the overall hygiene situation within the hospital. With no storage space for all those items, the space below the bed is used to store them—that is, as long as the space is not used for a short nap by a caregiver. In fact, moments of rest are rare. In these moments they sit and wait or dose off on the small uncomfortable wooden benches.
Their silent presence alone lends comfort to the sick. These caregivers’ lives are on hold, too, with all their time spent here. They remain with the patient from the moment they brought them in. In the meantime, other family members are required to give their indirect support as well: even if not actively involved at the hospital, they have to take over the care of children and/or elders, do the household chores and earn money. In the mornings, when the floor is mopped, all items are piled up on the narrow benches and people hold up their feet. When this is over, the sleeping mats and water bottles are stored underneath the bed and the daily bustle of moving between the nurse’s office and laboratory and the transportation of the sick to the ultrasound and X-ray rooms begins. After the first ward round, the nurses will hand out a variety of forms and handwritten notes. Everybody is on the move now—one of the caregivers will pick up empty containers for different body fluids. Once filled, the caregiver will take them to the necessary location, either to the nurse’s office or to a laboratory in another part of the hospital. Next, more forms are handed out to the caregivers. These forms will enable them to retrieve the necessary medication, which they will need to give to their sick relative. Handwritten notes are also handed out. They list additional medicine, which the family must buy at the pharmacy themselves and add to the pillbox on their own.
The nurses are responsible for injections, measuring body temperature and taking blood samples. A nurse is also responsible for installing the drip, but once it runs out the caregiver will be the one to remove it. Finally, if required, the caregivers will roll over the oxygen flask, attach it and regulate it. As soon as the most pressing tasks have been taken care of, the caregivers will move quickly to secure two bars that will hold up the mosquito net for the coming night. All other items must be brought from home: sheets, blankets, cushions, stools to sit on. Garbage bins must be brought, too, to serve as waste disposal and spittoon. Simple measures could certainly improve the overall conditions, such as mosquito nets for everyone, including the families sleeping on the floor; (anti-septic) soap in the bathroom; a cafeteria, which follows hygiene rules and is inexpensive (for free, at best) so that proper and balanced meals are available for everyone. At this point in time the amount of comfort provided to the patient solely depends on the financial and personnel capacity of the family. And it depends on family members having the educational background to understand the disease and which precautions—especially in terms of hygiene—are necessary for those around to follow to increase the chance of recovery and to avoid contagion.

Forging Alliances
Relationships between the different patients’ family members grow by the day. There is a general tendency for women to sit down and chat, while the male caregivers hang out at a bit of a distance, engaged in conversation and joking. Most tasks are done by caregivers regardless of their gender. In other situations, organizing meals and preparing tea are typical female tasks in Myanmar, but here they are done by all. The differences concerning gender lie in the small things: for example, carrying the heavy load of drinking water is a typical male task, and without further ado the men bring extra for bed neighbours whose caregivers are solely female. Any surplus is immediately redistributed amongst those families that have already spent one or two days together. This may be drinking water or food, which some visitors bring along. Indeed, food is the most important and the most appreciated gift in the hospital. And the redistribution of surplus is a marker of reciprocal material exchange. Another part consists of active support in caregivers’ tasks. Being constantly present is a prerequisite to carrying out one’s caregiving duties, but this is sometimes difficult to accomplish. In these instances, observant caregivers of neighbouring patients ensure that the patient’s needs are looked after when their own caregiver is absent. On some days, my friend’s mother-in-law, the daughter and granddaughter of our bed neighbour leave together to take a shower after lunchtime. The communal bathroom here is in an acceptable condition compared to some other hospitals. Taking a shower, however, remains tricky for patients. The facility offers only cold water (problematic for those suffering from infections, etc.), and the patients are required to get themselves there. Lastly, there is a financial obstacle, as each shower costs a hundred kyat. In the meantime it is my duty to watch over not only my friend but also the grandmother next to her, who is either deeply focused on her smartphone or crafting a bag made of tiny pearls. After their return, the male patient’s son from the bed across asks why they are not wearing thanaka[i]. It seems that a shower has not been completed if thanaka paste is not applied to the face. It was part of the plan anyway, as just then a mat is placed on the floor and a small kyauk pin (thanaka grinding stone) is taken out from a cosmetics bag. All three women apply a first layer of the white fluid mass on their face and add a second layer to their cheeks and forehead. The fact that their group is composed of three women, as is ours, is referred to repeatedly. I feel that in this way our mutual support is emphasized and communicated. By now our relations also extend to the bed neighbours on the right side. Two days ago a woman (visibly and audibly in pain) and her husband came in. He is a moto-taxi driver, but now his job has taken a backseat. Except for today, when my friend’s mother-inlaw, who is doing the twenty-four-hour shift in our case, needs to return to Sagaing to pick up medication at the hospital there. My friend’s initial treatment had started there but (for reasons not fully clear to me) cannot be continued here. This requires the regular collection of medication prescribed in Sagaing, a forty-five-minute motorbike ride from here. During their absence my caregiving duties automatically extend to include the taxi driver’s wife. It is not exactly easy—my Burmese language skills are unable to handle a hospital environment and body/pain/medicine-related issues. To my relief, her daughter arrives to take over. At the same time the nurses call us to pick up some of the medicine. The left bed neighbour’s granddaughter immediately comes over and takes our pill box— detecting my insecurity before I even realize it myself—and takes care of pill management for both patients. She comes back and explains when to administer them. I suspect that with all the other tasks and the occasional absences, an accurate schedule can barely be kept by anyone. Suddenly, an elderly lady sits down next to me and lets out a stream of words, which I can barely follow. It is unclear if she expects me to understand her. But when some question marks become evident, she turns to my ear and repeats everything very loudly. Suppressing my laughter, I reply in simple Burmese to show that this is my true problem, not deafness. Bit by bit I learn that she is a ka sayama, a Myanmar traditional dance teacher, and that it is her husband who lies in the bed across from us. It is the first time she has shown up, and as lively as she is I guess that being here is against her nature. She presents old photographs and explains in which cities she had taught dancing. She had even been to Eastern Shan State, so we chat a bit about my previous research area, Kengtung. She disappears as suddenly as she arrived, leaving her son to care for his father. Their son is in his mid-forties and a very good-natured person. This morning he ordered a second breakfast for my friend and shares our opinion that it is of utmost importance for her to regain ar—energy/strength.

Spheres Do Not Mingle
These encounters show that solidarity between people softens the hardships of inefficient management and resource allocation within the healthcare system. Used to patients’ complaints about long waiting times and crowded waiting rooms in Germany, I have learnt from the patience and appreciation of patients’ and carers’ attitudes towards the physicians. In a country with less than nine physicians per ten thousand inhabitants (World Health Organization 2019), physicians in Myanmar work hard indeed. The lack of access to medicine and laboratory tests, widely available in neighbouring countries, is one of the reasons why medical teams cannot work to the full extent of their capabilities, apart from their tiring long shifts. Their income is often too low to sustain themselves; most physicians run evening duties at private clinics in addition to their day job. Besides these trained medical professionals, knowledge about health and hygiene among the public remains limited. This results in an acceptance of the situation and no active inquiries or questions made to the physicians. In general, hierarchical order is adhered to in Myanmar, and it is no different in this context. As such, this order also prevents any scepticism towards the medical courses of action. The physicians’ authority is not questioned, and this can lead to oversight of symptoms, since patients and caregivers do not report symptoms that are not specifically inquired about by physicians. The alliances forged do not extend beyond the realm of patients and caregivers; the realm of nurses and physicians remains separate. Both realms coexist and are interdependent, but they only intersect during a few moments in time. The medical team does all in its power to find causes, order the necessary (available) tests and prescribe (available) medicine. The outcome is regularly checked with the patient. While this process takes place, all lives are on standby. The caregivers focus on the patient’s recovery and do all in their power to ensure it. As has been described, material exchanges and reciprocal duty provisions are the strategies deployed, rendering solidarity the central feature within this group.

Time for Goodbyes
Sooner or later the patients and their caregivers are sent home again. Depending on the time spent together, some people may keep in touch. Before parting, useful items like drinking water are redistributed and all belongings packed up. The metal bed frame with its blue plastic mat is all that remains, as if the whole setup of a temporary home had never existed. For the physicians and nurses working on my friend’s case, I was an added challenge. Although I was trying to adapt to Myanmar’s hospital culture, I could not always suppress impatience, critical questions or tears (making me the only one who cried at the ward, which made it very uncomfortable for those around). When my friend’s health stabilized, we left the hospital. But, because of her terminal illness, it was not long before she had to leave this world in an untimely manner, aged only thirty-one years. She is survived by two lovely boys, her husband and family.
[i] Thanaka is a paste derived from ground tree bark and water. It is applied to the face (and sometimes the body) as sun protection, natural skin lightener, makeup and for its cooling properties.
References
World Health Organization. 2019. Data Source: NHWA data platform 2018. http://apps.who.int/gho/data/node.main.HWFGRP_0020?lang=en (accessed 27 August 2019).
All photos were taken by Jella Fink in 2018.
Article was previously published in: Sojourn: Journal of Social Issues in Southeast Asia , Vol. 34, No. 3 (November 2019), pp. 646-659 Published by: ISEAS – Yusof Ishak Institute

Jella Fink is a cultural anthropologist specializing on material culture, minorities and rural economies in Myanmar.